With 2021 done and dusted, we’d thought we would look back at some of the emerging healthcare trends that will follow us into 2022. As Omicron cases surge, it’s clear that COVID-19 isn’t going away just yet. If anything, we can expect more of the unexpected in 2022.
Here are a few trends that we expect to follow us into the new year:
Shifting care from hospitals
Hospitals are no longer the epicenter for patient care. Both physician groups and ambulatory surgery centers have seen an increase in the number of procedures taking place.
Shifting care to physician groups
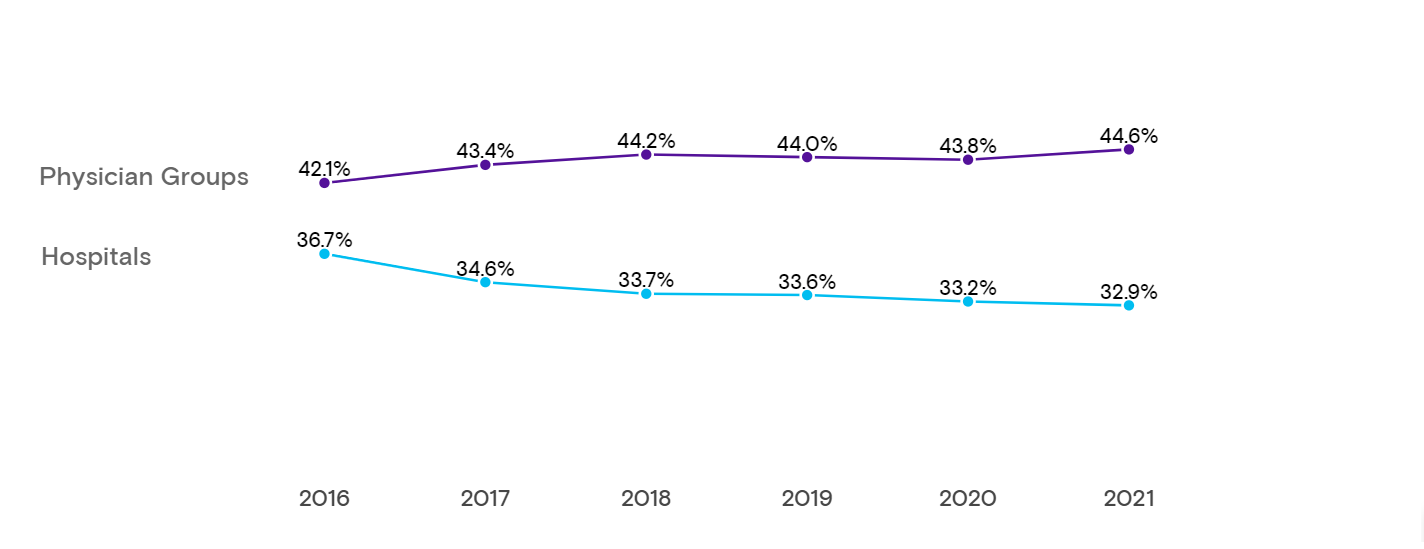
Less than a third of the 2.4 billion procedure claims tracked by Definitive Healthcare through the end of November 2021 came from a hospital facility, down from 38.7% in 2016. Meanwhile, procedure claims for physician groups accounted for 42.1% of claims in 2016 and increased to 44.6% of claims in 2021.
COVID-19 doesn’t appear to be entirely to blame for this shift, as physicians group visit volume – in other words, physicians treating patients at non-hospital locations – has been on a slow uptick since before the pandemic hit.
Diagnosis and procedure claims by facility type from 2016-2021
Fig 1. Data from Definitive Healthcare’s ClaimsMx product. Data represents the change in the share of the total diagnosis and procedure claims by facility type for physicians groups and hospitals between 2016-2021. Commercial claims data is sourced from multiple medical claims clearinghouses in the United States. Data is updated monthly; accessed January 2022.
Shifting care to ambulatory surgical centers
We’re also seeing procedure volume at ambulatory surgical centers grow quickly.
By November 2021, 14.6 million patients had a procedure at an ambulatory surgery center this year. While volume dropped due to the pandemic, ambulatory surgery centers regained nearly 94% of patient volume in 2021 compared to 2019.
Pre-pandemic, we saw the procedure volumes at ambulatory surgical centers grow faster than at hospitals.
Between 2016 and 2019, the number of patients that had a procedure at an ambulatory surgical center increased by 16%. Meanwhile, patients who had a hospital procedure increased by only about 6%.
Since ambulatory surgical centers offer patients high-quality care at lower costs, they are an attractive alternative for patients requiring outpatient care. We expect to see volume increase at ambulatory surgical centers in 2022.
Remote patient monitoring continues to grow
While telehealth’s explosive growth dominated the conversation at the start of the pandemic, remote patient monitoring experienced its own triple-digit explosive growth in 2020.
What is remote patient monitoring?
Remote patient monitoring (RPM) is a newer method of care delivery that leverages technology to monitor and gather clinical data on patients outside of a traditional clinical care setting.
RPM typically uses digital technology to capture physiologic healthcare data from patients and electronically transmits it to healthcare providers for assessment. Some common RPM devices include blood pressure monitors, blood glucose monitors and weight monitors.
Remote patient monitoring setup increased nearly 40% compared to 2020
CMS outlines the four codes below as the primary codes to bill for remote patient monitoring services.
According to our ClaimsMx data, the procedure volume for all codes increased compared to 2020. The initial setup and onboarding of a patient to an RPM device (CPT 99453) increased nearly 40% compared to 2020 and nearly 572% compared to 2019.
Unlike telehealth, which has seen adoption plateau, it appears remote patient monitoring is continuing to gain in popularity, and there are still many opportunities for its use in the management of chronic conditions.
Remote patient monitoring procedure volume 2020-2021
| CPT Code | Description | 2020 Procedure Volume | 2021 Procedure Volume | Percent Change |
| 99453 | Remote monitoring of physiologic parameter(s) (eg, weight, blood pressure, pulse oximetry, respiratory flow rate), initial; set-up and patient education on use of equipment | 63,595 | 88,599 | 39.3% |
| 99454 | Remote monitoring of physiologic parameter(s) (eg, weight, blood pressure, pulse oximetry, respiratory flow rate), initial; device(s) supply with daily recording(s) or programmed alert(s) transmission, each 30 days | 235,714 | 464,442 | 97% |
| 99457 | Remote physiologic monitoring treatment management services, 20 minutes or more of clinical staff/physician/other qualified healthcare professional time in a calendar month requiring interactive communication with the patient/caregiver during the month | 191,310 | 474,076 | 147.8% |
| 99458 | Remote physiologic monitoring treatment management services, clinical staff/physician/other qualified health care professional time in a calendar month requiring interactive communication with the patient/caregiver during the month; each additional 20 minutes (list separately in addition to code for primary procedure) | 56,345 | 155,781 | 176.5% |
Fig. 2 Data from Definitive Healthcare’s ClaimsMx product for the calendar year 2020 and 2021 (through November 2021). Commercial claims data is sourced from multiple medical claims clearinghouses in the United States. Data is updated monthly; accessed January 2022.
Staffing shortages and an aging workforce
Thanks to the Great Resignation, staffing shortages are hitting every industry, and now Omicron is exacerbating issues.
According to the Association of American Medical Colleges (AAMC), the U.S. could see an estimated shortage of between 37,800 and 124,000 physicians by 2034.
Healthcare is facing massive physician and nursing shortages due to a wide range of reasons, ranging from providers falling ill with COVID, to practitioners leaving the practice of medicine altogether due to overwhelming burnout.
The problem isn’t going to get better anytime soon.
According to data from PhysicianView, the average age for providers is 53 years old. Cardiac surgeons and general practice physicians tend to be a bit older, coming in with an average age of 58, while hospitalists are younger with an average age of 43.
Many physicians will be nearing retirement in the coming years, with some opting for early retirement due to COVID, which could worsen hospital staffing shortages in 2022 and beyond.
Elective surgery starts and stops
COVID-19 caused a chaotic year for elective surgeries. As COVID cases spiked with the Delta and the Omicron variants in late-2021, many hospitals were forced to postpone or cancel elective procedures once again to free up resources.
However, it is not all bad news. Early in 2021 when COVID-19 case numbers remained low, hospitals were able to reopen their doors for elective surgeries and restore volume for some procedures to near 2019 levels.
For example, total knee and hip replacement surgery volumes through November 2021 are 92% and 98% of 2019 volumes, respectively.
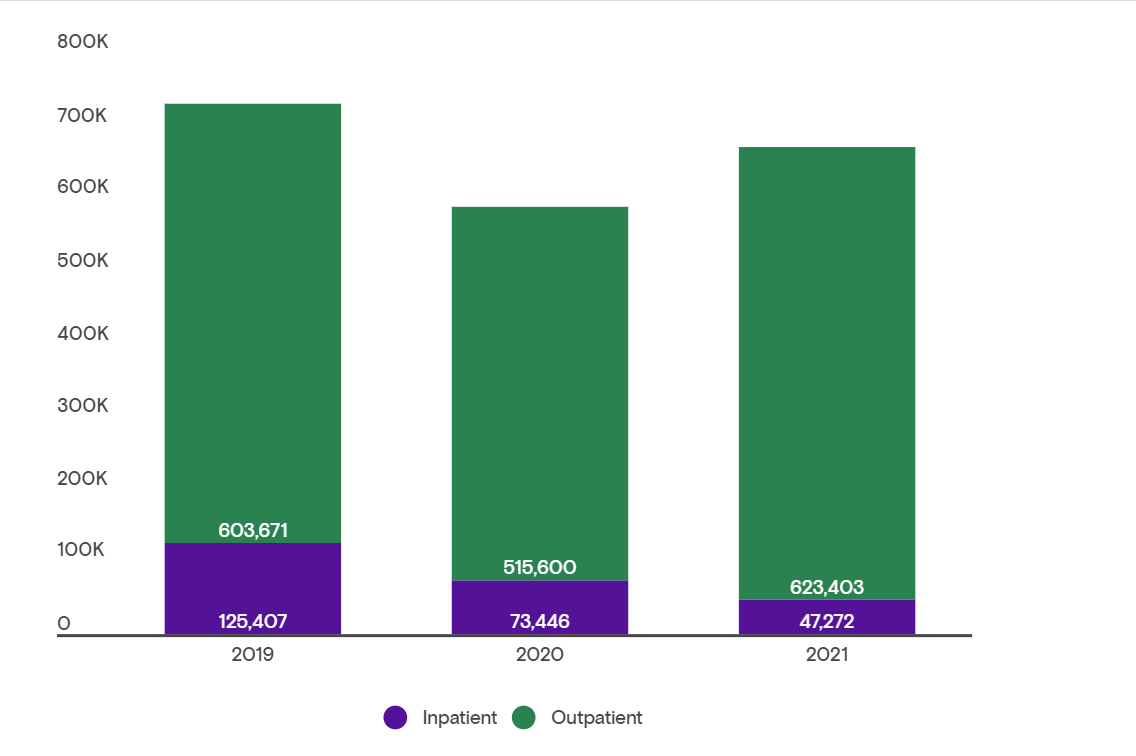
Knee replacement inpatient vs. outpatient procedures 2019-2021
Fig 3. Data from Definitive Healthcare’s ClaimsMx product. Commercial claims data is sourced from multiple medical claims clearinghouses in the United States. Data is updated monthly; accessed January 2022.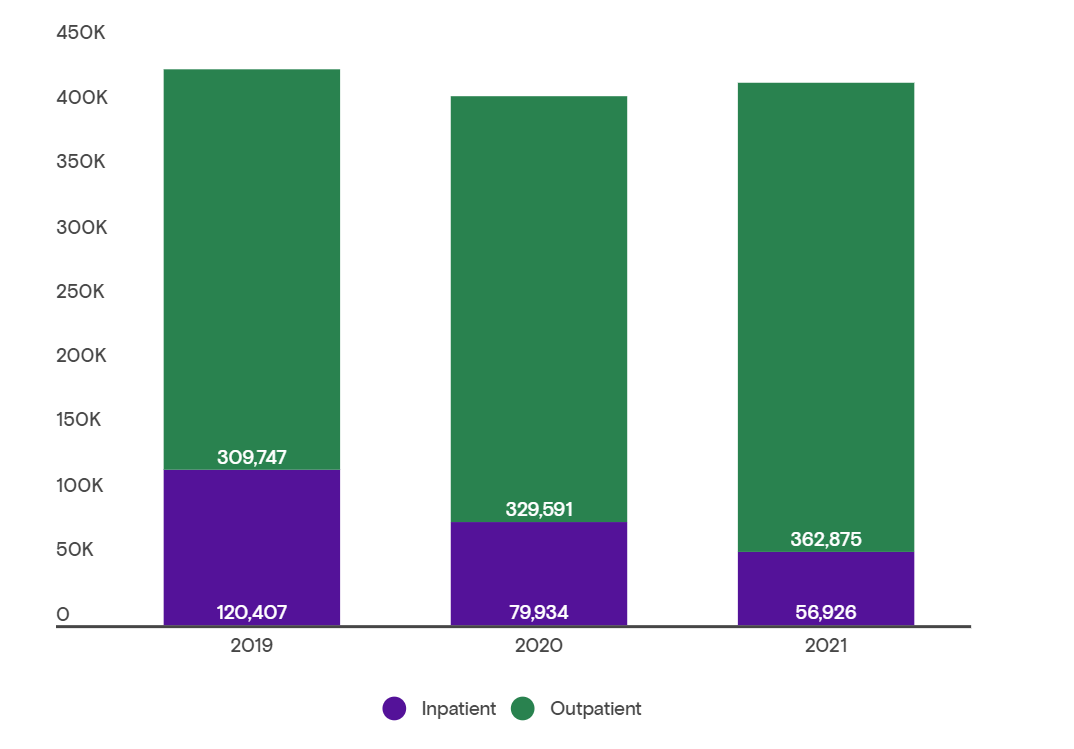
Hip replacement inpatient vs. outpatient procedures 2019-2021
Fig. 4 Data from Definitive Healthcare’s ClaimsMx product. Commercial claims data is sourced from multiple medical claims clearinghouses in the United States. Data is updated monthly; accessed January 2022.
For both types of surgeries, procedures performed on an outpatient basis increased from 2019, while inpatient procedures have dropped. Most of these procedures have always taken place in an outpatient setting. However, the decrease in inpatient procedures could be due to the postponement of elective procedures as COVID cases rose.
Drug charges decline while drug costs remain high for patients
High drug prices continue to make the headlines. According to a 2021 Gallup poll, an estimated 18 million Americans cannot pay for needed drugs.
However, according to our ClaimRx data, overall charges for prescription drugs are down slightly compared to 2020 and 2019. Through the end of October, we’ve recorded over $134.4 billion in drug charges in 2021. That’s a slight decrease from $149.2 billion in 2020 and $154.9 billion in 2019.
Now it is important to note that these numbers are prescription charges. They do not represent the price a patient would pay at the pharmacy. The numbers represented here are the amount charged to insurance companies each year. The amount a patient pays for a prescription depends on various factors and patients rarely pay the list price for a drug if they have insurance.
In addition to a slight decrease in total drug charges, the average prescription charges by state dropped to $2.4 billion in 2021, compared to $2.7 billion in 2020 and $2.8 billion in 2019.
Overall drug charges are likely down because of delays in care over the last two years. Fewer patients visiting the doctor mean fewer drugs getting prescribed and fewer prescriptions getting renewed.
Additionally, the pandemic resulted in millions of Americans losing their jobs, resulting in added financial hardships and the loss of their health insurance. This likely also contributed to the slight decline in overall drug charges since 2019.
___
The post was originally published on the Definitive Healthcare blog.