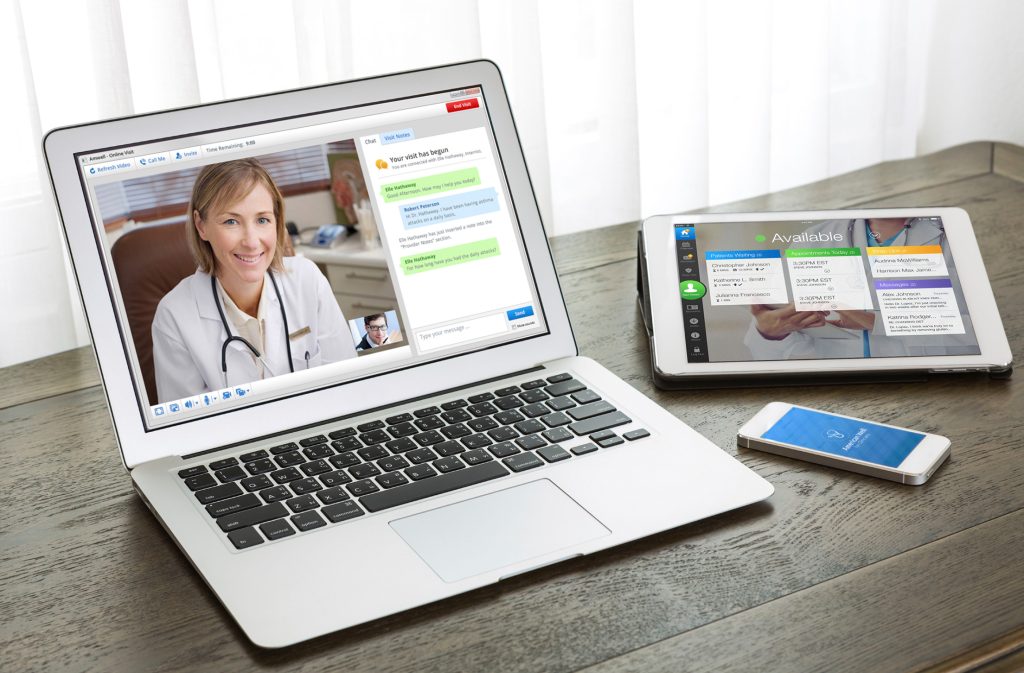
For Amwell, making healthcare accessible to all has always been core to their mission, but it was the global pandemic that brought that once unique mission mainstream. When healthcare providers were forced to radically transform the way they do business, Amwell was ready with over 15 years of telemedicine and virtual care delivery experience to share.
 In a year when healthcare had unprecedented and mission-critical needs, Amwell responded. For this reason, MassTLC honored Amwell this year with a Tech Top 50 award for “Business Accomplishment.”
In a year when healthcare had unprecedented and mission-critical needs, Amwell responded. For this reason, MassTLC honored Amwell this year with a Tech Top 50 award for “Business Accomplishment.”
Jon Bernstein, New England Regional President at PNC Bank, – a Tech Top 50 Platinum Sponsor- recently joined Mary Modahl, CMO of Amwell, for a conversation about the company’s unlikely trajectory, its core vision, and what’s next.
Tech Top 50 Platinum Sponsor- recently joined Mary Modahl, CMO of Amwell, for a conversation about the company’s unlikely trajectory, its core vision, and what’s next.
For Modahl, who has been with Amwell for nearly a decade, one thing is certain in these uncertain times: even beyond Amwell, transformations in digital care will change the way care is delivered forever – and that is a very good thing.
___
Jon Bernstein: Congratulations on the success of Amwell over the last couple of years. It’s been an amazing trajectory, what you’ve done. For those who don’t know about Amwell, could you please tell us a little bit about the company?
Mary Modahl: Amwell is a digital health company, and we are focused on virtual care delivery. We work with major hospitals, healthcare delivery systems, and health plans to design and develop virtual health care. We’ve been in business for over 15 years here in Massachusetts, and we work with most of the top brands in the business. We are an infrastructure technology, if you will. We help leaders that have established their presence in the healthcare space over the past 100 years to modernize and become digital in the way they deliver healthcare. We’re not a disrupter that looks to replace the major hospital systems and health plans. In fact, we’re an enabler to those players. We offer a real breadth and depth of services when it comes to virtual care.
Typically, you can think about virtual care in three broad categories. One is on-demand types of episodic care, and this can include urgent care, but it also can include episodic care like strokes. The second type is longitudinal, scheduled types of care. For example, folks that might be struggling with a chronic condition or cancer, and they may need individual providers, or even an entire care team, for care that takes place over time. The third type is provider-to-provider. For example, you might have a hospital in a more rural area, and for highly complicated or specialized cases, they might want to bring in specialists from the major academic medical center. We power all of these digital care interactions. This breadth of digital care delivery is really what Amwell is all about. We work with a lot of the big players in healthcare, and we’re honored to do so.
Jon: How has COVID upended the delivery and the utilization of your products? What have you seen in the last 18 months?
Mary: It’s been a huge shift, Jon. Before the pandemic, virtual care was kind of an experimental field. There were some applications that were pretty widely deployed, specifically urgent care, and telestroke, along with some virtual behavioral healthcare. What really changed during the pandemic is that, all of a sudden, people needed to be at home, and hospital systems were struggling with very ill COVID patients, and they really needed to protect all other patients from exposure to this disease, particularly in its earliest iteration. Very rapidly, every provider in the country had an experience with virtual care.
Before the pandemic, only 8% of providers—meaning doctors, nurses, other clinicians—had ever done virtual care. After the pandemic, 94% have done it. It’s a huge experience difference for people who are in healthcare delivery, and it allows the clinical workforce to really take stock of the possibilities of this technology, in terms of longitudinal care, reporting, reducing administration, and enabling different locations for providers. It was really an eye opener on the clinical side. Same thing on the patient side. Have you seen your doctor virtually in the last year, or any other clinician?
“Before the pandemic, only 8% of providers—meaning doctors, nurses, other clinicians—had ever done virtual care. After the pandemic, 94% have done it.”
Jon: We’ve seen other clinicians virtually. Yes.
Mary: Most people have, and before the pandemic, most people hadn’t. I think, particularly when you combine that with the changed expectations that we see generationally, millennials and even younger individuals are coming from the point of view of, “Well, if I could do this on my phone, why wouldn’t I?” There are always going to be things in healthcare that have to be done in person. Surgeries are going to be surgeries, but what if follow-up can be done right in the home? What if we can have a wound-care specialist look at a wound alongside a spouse, who’s trying to take care of you after your surgery? It’s really transformative to the mindset that people have, and I think that’s the biggest single change that happened in our field as a result of the pandemic.
Jon: The return on investments for the providers in working with you must be great. In terms of the utilization of their clinicians, their wait times can go down, the number of people they can see can go up. Have you actually been able to see an increase in the volume and capacity of systems?
Mary: It’s been gigantic. We saw average monthly visits and average monthly active providers delivering healthcare on our platform increase over 300% and 400%, respectively between Q1 of 2020 and Q2 2020, during the beginning of the pandemic. In terms of the value to healthcare providers, it has enabled them to deliver scarce resources (for example, outside of exclusively major metropolitan areas to rural areas), and this has really changed the way healthcare systems can think about delivering care.
Patient acquisition has changed a lot too. We used to think about our catchment area in terms of drive time. How far can you drive? What patients could you serve based on how far they had to drive? Now, there’s both the ability to say, “Okay, well, actually, we could serve an entire region, or we might even have national services that we could provide.” That’s the beginning of a real mindset shift in healthcare delivery. It’s exciting.
Jon: With the ability for a patient to access healthcare virtually now, has that changed the competitive buying power between the patient or the supplier in medicine?
Mary: We used to be in pretty much exclusively geographic markets, with some services that people would travel for inside and even outside the U.S., but I think a lot of healthcare is actually hybrid. It needs to be both virtual and physical. I think we’re seeing the emergence of competitiveness on a digital stage for healthcare delivery but combined with a physical element too. This is hybrid care, and Amwell is a significant enabler of these kinds of programs for hospital systems.
Healthcare is not like finance, which can be entirely virtual. People still need to see people in-person in healthcare, and they want relationships that are physical, but it’s likely that there will be care pathways that combine elements of both physical and virtual.
Jon: What’s really amazing with Amwell is how it has been able to connect to customers virtually and meet clients where they need to be met. Up until this point, it has been challenging for healthcare to evolve into this delivery model, but Amwell has been able to facilitate the transformation. Did you recognize that that’s where Amwell would take healthcare in the modern age? Was this part of the original vision?
Mary: It has always been the vision of Amwell, always. We were evangelizing for many years. Our founders, Roy and Ido Schoenberg, call it “the years in the desert.” We were there evangelizing alone for a long time. Certainly, there was big growth all the way through the process, but the pandemic really did shift things. I think back to when the New York City healthcare system became really overwhelmed with its emergency medical system. Too many people, some of whom were really ill, and some of whom were just worried, were calling ambulances. The ability to come in and help them triage that virtually was huge.
People had experiences and eye-opening moments during the pandemic about what virtual care might mean. We’re right now still at the very beginning. Once people’s minds’ eyes have opened to what something might mean, then begins a real acceleration. Amwell is not alone in this anymore. Everybody is talking about virtual care. It’s a big thing, and that’s an exciting shift.
Jon: You’ve had the vision for a long time, and the pandemic accelerated the acceptance of it. Where does Amwell go? What does the future hold?
Mary: The biggest thing that we’re doing right now is rolling out our new Converge platform. During the peak of the pandemic, we were at 10x volume daily. It was gigantic. We had hospital systems that were piloting with five providers on March 12th, 2020, and on March 20th of 2020, they asked us if they could stand up 500 providers on the system. It happened like that for us. We had such an acceleration, and we learned a ton about the scalability and the modularity of the system and the range of services that could be done. Hospital systems called us with use cases that we’d never thought of before, because, all of a sudden, they had new problems they had to solve.
Converge is our response to our new understanding of what virtual care and digital care can be. It combines virtual care visits with many more automated aspects of care, things that can be done by computer systems working with people to move things along, to streamline them, to make them more efficient, and at the same time, more continuous and more effective.
I’ll give you one example. We’ve been working on translation services. My daughter is an emergency room physician, and she probably has between 5 and 10 different languages come through her ER every single day. How do we handle something as simple as translation, so that I can speak in my native language, you can hear in your native language, and we can have a good healthcare conversation? These kinds of technologies are incredibly exciting in healthcare, and really could be gamechangers.
People who speak languages other than English suffer significant access gaps. People who don’t live in metropolitan areas where there are academic medical centers have significantly less access to medical expertise than other people who do. The ability to transcend these boundaries is one of the big promises of virtual care, and I think it’s an incredibly exciting mission.
Jon: Have you been able to expand access to communities that beforehand had been challenged?
Mary: Absolutely. There’s been a very significant federal grant program in this area, because, all of a sudden, during this recent pandemic experience, there was the realization that many people really couldn’t get into or didn’t have access to healthcare. This Infrastructure Bill, with its extension of broadband into rural areas of the United States, is a very significant development for the expansion of telehealth, as are 5G networks on the cellular network. A lot of these areas are in the Western US, but we have rural areas in Massachusetts too. We have big swaths of rural areas in Maine, New Hampshire, Vermont, and all the New England states have significantly less-accessible areas.
It has been a major part of what we’ve always done. We’ve always had carts in school systems in rural areas that allow school nurses to connect with a clinician in the hospital system. We always supported the rural healthcare location that wants to have a provider-to-provider connection for a telestroke or a neurology consult or a cardiology consult. I think now there is a huge change afoot across the delivery system coming out of the pandemic that I think is going to significantly increase that access, both for rural versus urban, as well as different types of people, based on their culture, language, etc.
Jon: What does it mean for Amwell to be recognized in the MassTLC Tech Top 50? What comes next?
Mary: It means the world to us. We’re really humbled and really honored by it. For us, it’s an exciting moment, because I think a lot of people who were in tech during the pandemic have stepped back to say, “Gee, what am I doing with my life? How am I spending my time? What am I contributing to my world and my society?” If you’re in tech, digital health and virtual care really aligns the need for significant, advanced, exciting, leading-edge technical development with a humanistic mission, where the product is there to help people, and it demonstrably does. For us, that’s the big thing about the MassTLC recognition. We really appreciate that this is coming to the forefront.
And we’re growing. We’re seeking people. If you’re looking for exciting leading-edge technology and also a mission that matters to humanity, I urge you to look at digital healthcare and come look at Amwell. We’ve all had personal experiences at a deep level in the last year. Each of us has been on a personal journey alone in our living room, or wherever we were, to ask what it all means. I think now more than ever, it really matters to work in an area that gives back.
Jon: We’re thrilled to be able to recognize you. Thank you for the great vision and success that you’ve had over the time, and for being persistent for as long as you have.
Mary: I’m excited about where Amwell is headed and where virtual care delivery is headed. Before, it was sort of the odd innovator type who really looked at virtual care. Now, it’s going mainstream, and it’s changing the clinical conversation in profound ways. I really mean it when I say it’s just the beginning. Digital care delivery is going to be very transformative over the next 10 to 15 years. Even beyond Amwell, I’m quite optimistic about what’s coming in healthcare.
“it’s just the beginning. Digital care delivery is going to be very transformative over the next 10 to 15 years.”
___